A visual field test is preformed by a specially trained technician. The results of each individual eye are registered in print and the patient is requested to give the test results to the ophthalmologist during the patient’s next visit. According to the findings in the test, the doctor can diagnose the patient, and determine what the best treatment is.
A visual field test is preformed by a specially trained technician. The results of each individual eye are registered in print and the patient is requested to give the test results to the ophthalmologist during the patient’s next visit. According to the findings in the test, the doctor can diagnose the patient, and determine what the best treatment is.
How does the doctor determine the diagnosis from the information acquired during a visual field test? Interpreting the results of this test is not an easy task, and it can take doctors who specialize in ophthalmology a few months to learn how to accurately interpret the different information appearing on the printout.
The printed page summarizing the results of the test includes a map composed of different shades, accompanied by various mathematical calculations and statistical analyses, enabling your physician to visualize any defects in your visual field. The map, which is composed of diverse shades, is located on the upper right-hand side of the printout and next to it, on the upper left-hand side, are various numerical calues that are directly related to the varying shades seen in the map. The map of shades is relatively straightforward and easy to understand; the lighter shades represent healthy retina while the darker shades correspond to the areas in the retina that suffer from damage caused by glaucoma. Regions that are completely black denote portions of the retina that did not detect even the strongest light given off by the device. Therefore, the darker areas in the map, in particular the black ones, denote the parts of the retina in which sensitivity to light has deteriorated significantly.

It is important to remember that each eye (both healthy and sick) has a “blind spot”. This is an area of the retina that does not see, and is anatomically the area in which the optic nerve exits on the retina. This area is represented on the visual map as a black round spot, slightly smaller then the size of a 1 shekel coin, located slightly to the left or to the right (depending on the eye) of the centre of the visual field. Occasionally a healthy patient of mine arrives worried, pointing out to me the “damage” seen in their visual field, which is no more than a normal ‘blind spot’.
Why is one visual test not enough?
 During the test light is projected onto a screen in order to measure the sensitivity of different parts of the retina to light. The patient is asked to press a button when he observes a light. During the examination the light shined changes intensity, and is often very dim, to the point that it is undetectable by the patient’s eye. The device can then calculate the minimal intensity of light that a patient can actually see, a separate value for each part of the visual field. The test is preformed separately for the right, and for the left, eye. This is a long, boring and stressful test, requiring intense concentration over an extended period of time. It is therefore dreaded and hated by most patients. If you feel this way, you should know that it is the normal reaction of most, if not all, patients. In addition, a large majority of patients, whether healthy or sick, constantly feel that they have preformed poorly on the test. Some feel anxiety and frustration from not seeing the light properly and some feel that their vision has deteriorated since the last test. It is important to explain to these individuals that these feelings are normal reactions to the test, and shared by both sick and healthy patients alike and is due to the fact that during the test the light projected on the screen slowly decreases in intensity, until it becomes harder and harder to detect until completely undetectable. No matter what your vision is, most lights shined during the test will be, by definition, almost impossible to detect.
During the test light is projected onto a screen in order to measure the sensitivity of different parts of the retina to light. The patient is asked to press a button when he observes a light. During the examination the light shined changes intensity, and is often very dim, to the point that it is undetectable by the patient’s eye. The device can then calculate the minimal intensity of light that a patient can actually see, a separate value for each part of the visual field. The test is preformed separately for the right, and for the left, eye. This is a long, boring and stressful test, requiring intense concentration over an extended period of time. It is therefore dreaded and hated by most patients. If you feel this way, you should know that it is the normal reaction of most, if not all, patients. In addition, a large majority of patients, whether healthy or sick, constantly feel that they have preformed poorly on the test. Some feel anxiety and frustration from not seeing the light properly and some feel that their vision has deteriorated since the last test. It is important to explain to these individuals that these feelings are normal reactions to the test, and shared by both sick and healthy patients alike and is due to the fact that during the test the light projected on the screen slowly decreases in intensity, until it becomes harder and harder to detect until completely undetectable. No matter what your vision is, most lights shined during the test will be, by definition, almost impossible to detect.
Most patients will be more than happy to skip this test, but it is an essential part of your examination since it provides crucial information, initially for the diagnosis of the disease and later to assess whether progression had occurred. Therefore, it is crucial that patients continue to undergo these tests as often as the doctor requests them. The frequency in which the test will be required may vary between once every few months and up to once a year or so, according to the severity of the disease, the intra-ocular pressure and additional factors.
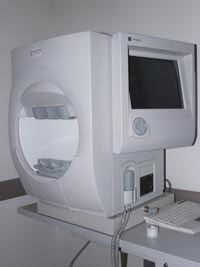 It is important to be aware of the fact that with time, new computer algorithms are constantly developed, recently employing artificial intelligence. These algorithms residing inside the visual field machine, which is a computer, shorten the length of the test without cutting back on its accuracy. Today both eyes can be tested in the same amount of time it previously took to test just one eye.
It is important to be aware of the fact that with time, new computer algorithms are constantly developed, recently employing artificial intelligence. These algorithms residing inside the visual field machine, which is a computer, shorten the length of the test without cutting back on its accuracy. Today both eyes can be tested in the same amount of time it previously took to test just one eye.
Glaucoma experts predict that in the very near future new technology will enable imaging of the ocular nerve and retina, imaging which would augment the information given by the visual field test. Consequently, the frequency of visual field tests required from the patient will decrease significantly. It is interesting to point out that while the visual field test is subjective and analyzes visual function, such imaging tests are objective in nature, and check anatomical structure as well as tissue damage. Therefore it is not hard to see how these two tests might complement each other and add crucial information regarding the existence (or lack of) and progression of this chronic, visual threatening disease, glaucoma.
Further information regarding the visual field test, see the following chapter:‘Deterioration of the visual field in glaucoma’.